Abstract
Irritant diaper dermatitis (IDD) is the most common dermatosis of the diaper area. Half of all infants experience some form of IDD in the first 12 months of life as a result of skin barrier damage due to contact with urine and faeces. Infant skin, although providing a competent barrier under basal conditions, is easily damaged when stressed by irritants, compared to older children’s skin. Furthermore, the skin of small infants is structurally and functionally immature compared to older children, with increased permeability to water, a higher pH and increased permeability to irritants and allergens. Improvements in the performance of disposable diapers and skin care have resulted in a substantial decrease in the prevalence and severity of IDD. However, despite these improvements, IDD remains a common problem. Treatment for IDD mainly comprises frequent diaper changes, gentle cleansing and the application of a barrier ointment, which coats and protects the stratum corneum. The IDD management paradigm has shifted from treatment towards prevention. However, traditional barrier ointment treatments have been often less than ideal for repeated application to the immature, fragile skin of infants. An IDD and atopic dermatitis expert panel recently reached a consensus on nine standards for the ideal IDD barrier formulation, including the need for it to be clinically tested in infants and to only include components with demonstrated safety and efficacy. This review provides an overview of the IDD literature, focusing on IDD pathophysiology and management, and gives the IDD expert panel’s consensus views on an ideal IDD topical preparation.
INTRODUCTION
The structure and function of the skin of a young healthy infant (<12 months) are immature compared to older children1,2,3. This immaturity is likely to contribute to predisposing young infants’ skin to the development of irritant diaper dermatitis (IDD). IDD is the most common inflammatory dermatosis seen in the diaper area of young infants4. Onset of IDD is generally between the first 3–12 weeks of life, with peak prevalence at 9–12 months4. It is a form of irritant contact dermatitis caused by the interaction of several contributory factors, the most important of which is repeated exposure to a combination of urine and faeces. The incidence and severity of IDD correlates with age and the frequency of bowel movements, in particular with diarrhea4,5,6,7. Other factors contributing to the development of IDD include the use of soaps/detergents, inappropriate topical therapies, systemic antibiotics and allergic reactions to diaper components and topical applications.
It has been estimated that approximately 50% of infants will experience a mild form of IDD during the first year of life, while 20% will experience moderate IDD and 5% severe IDD4,5. In recent years however, the incidence and severity of IDD appears to have decreased for several reasons, including improvements in diaper design and improved infant skin care8,9,10,11,12. The regular application of barrier ointments is recommended as part of the standard management of IDD13. However, the optimal composition for such emollients for use on an infant’s delicate skin has rarely been considered in the literature6. Numerous products and alternative therapies containing a range of chemicals, some of which could cause direct irritation or a risk of allergic sensitization, are available for the management of IDD14,15. Consequently, as IDD becomes less prevalent and severe, the focus of IDD management has gradually shifted towards prevention rather than treatment. However, currently available preparations have been developed from a treatment perspective and are not necessarily optimal for IDD prevention.
This review will provide an overview of the IDD literature, focusing on its underlying pathophysiology as well as current treatment and management strategies. Differences in skin structure and function that make infants (<12 months) more susceptible to IDD in comparison to older children (>12 months) will also be highlighted. Finally, the consensus outcomes of an expert panel meeting on best practice in IDD and atopic dermatitis (AD) management will be discussed.
DISTINCT SKIN STRUCTURE OF YOUNGER INFANTS
Infant (<12 months) skin is structurally and functionally different to that of older children (>12 months), and adults2. The main visible difference in infant skin is that the stratum corneum (SC) appears to have a denser network of microrelief structures (Figure 1).
Figure 1. Differences in the structure of infant skin2,3
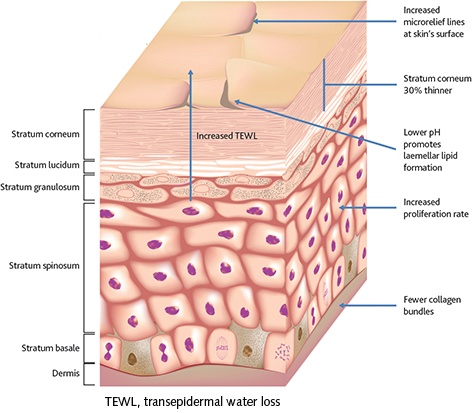
The SC and the epidermis of infants are thinner than those of older children and adults by 30% and 20%, respectively (Figure 2)2. However, infant skin has several features that support its development and maturity during the first year of life, including a higher proliferation rate, which aids the rapid maturation of the skin barrier (Figures 2)2. The slightly higher pH of skin at birth rapidly decreases in the first months, enhancing the formation of lamellar lipids and subsequent SC maturation. Lamellar lipids also facilitate repair of the skin barrier following disruption and/or injury2,3,16. Finally, infant skin has a higher natural water content than in older children, resulting in a somewhat higher transepidermal water loss (TEWL), but also promoting normal skin hydration (Figure 3)1. These features suggest that infant skin is structurally and functionally different from that of older children and might therefore be less able to withstand external irritant stresses.
Figure 2. Relative size of skin structures in infants and adults (A) Skin thickness; (B) Corneocyte size; (C) Granular cell size; (D) Granular cell desnity2

Figure 3. Differences in transepidermal water loss (TEWL) measurements, made using the closed chamber technique and a Delfin VapoMeter of infant and adult skin1

CAUSES OF IDD
IDD is a form of irritant contact dermatitis occurring in the diaper area. It is a multi-factorial disease, occurring as a result of several chemical irritants interacting with one another on the external surface of the skin6. The most important factor in the development of IDD is prolonged skin contact with urine and faeces. The urine/faeces mixture causes disruption of the skin barrier through several mechanisms, including maceration (softening by sustained wetness, swelling of corneocytes, and extraction of SC lipids and natural moisturizing factors), increased alkalinity, activation of faecal digestive enzymes and friction.
Maceration leads to disturbance of the skin barrier, in part due to the increased absorptive nature of infant skin, and results in the disruption of intercellular lipid lamellae17. A macerated SC shows heightened susceptibility to physical damage by friction, which may be caused by wipes or interaction with the diaper18. A local increase in alkalinity results from the deamination of urine to ammonia catalyzed by faecal ureases. This change of pH enhances the activation of faecal proteases and lipases, leading to digestion of skin lipids and proteins, causing irritation8,19.
Other irritant agents can cause IDD, such as soaps and detergents in high concentrations, which disrupt skin lipids. Allergens can penetrate into the skin and stimulate immune reactions and subsequent inflammation. Inappropriate topical treatments containing fragrances or preservatives may increase the risk of irritation and sensitization. In addition, frequent wiping and cleaning of the diaper area can also disturb the skin barrier, introducing irritants into the skin and causing further damage.
The pathology of IDD has not been shown to have a bacterial/fungal component at its inception6. However, systemic antibiotics and increases in pH have been documented to promote secondary infection in existing IDD cases, usually by disturbing the skin’s normal microflora and allowing colonization by opportunistic micro-organisms such as Candida albicans20.
MANAGEMENT OF IDD
Three steps should be taken in the management of IDD: gentle cleansing, immediate changing of diapers containing urine and faeces, and regular application of a protective barrier cream. These practices constitute good routine skincare, and should be implemented, especially in infants, preventing not only the occurrence of IDD but also other skin conditions, such as AD and contact dermatitis21.
Gentle Cleansing
The diaper area should be cleaned gently to remove irritants such as urine, faeces, and faecal enzymes. Excessive scrubbing should be avoided as this damages the stratum corneum. The use of substances with high alkalinity or detergent (lipid-removing) properties is not recommended. Instead, the use of infant wipes has been suggested to be more effective than water/mild detergent due to their ability to effectively remove lipophilic substances and buffer pH22,23. Following washing, skin should be gently patted dry e.g., with a soft towel, in order to avoid rubbing.
Good Diaper Practice
Diapers should be regularly changed to prevent prolonged contact of urine/faeces with the skin and thereby avoid unnecessary irritation. Use of disposable diapers is advised as they contain absorbent components, such as hydrocellulose gel, which are excellent at preventing urine from soaking into an infant’s skin.
Barrier Ointments
The use of barrier ointments containing moisturizers and products that enhance skin barrier function is encouraged9. However, the application of agents containing antiseptics is discouraged as they may disrupt the natural protective bacterial flora of the skin24.
STANDARDS OF AN IDEAL TOPICAL FORMULATION FOR IDD
Barrier ointments are becoming increasingly important as a means of IDD prevention. Given the differences between the skin of infants (<12 months) and older children (>12 months), the ideal composition of a topical IDD treatment has not yet been determined or developed, as shown by the wide range of formulae and ingredients used in currently marketed products. In June 2012, an international expert panel of dermatologists and pediatricians convened in London to discuss the optimal management of IDD. The meeting was an update of a previous meeting held in 2003 and the panel reviewed and reached consensus on the standards for an ideal topical formulation for IDD. The panel revised an earlier consensus published in 200420, increasing the previous seven standards to nine, which are discussed in the sections below (Table 1).
Table 1. The nine standards of an ideal irritant diaper dermatitis (IDD) preparation

Proven Clinical Efficacy and Safety in Babies
Within the European Union (EU), cosmetic formulations are tested for safety and efficacy in adults. However, complete cosmetic formulations do not need to be tested in infants or children <3 years if the individual components are demonstrated to be safe25. Ideally, any topical IDD preparation should be tested for efficacy and safety in this age group.
Enhances Natural Protection of the Skin
Key properties of an effective IDD preparation are protection of the skin barrier and promotion of skin repair, in order to help minimize contact with irritants and resulting skin damage. In addition to emollients, which provide a barrier between the skin and external environment, skin care agents such as dexpanthenol, nicotinamide and phospholipids have also been shown to enhance the production of natural lipids and to reduce signs of irritation, aiding in the repair of the skin barrier26,27,28,29. Enhancing the production of natural lipids is advantageous, as topical creams and ointments can only mimic the natural lipid content of the skin, which contains a very complex mixture of lipids, including several different ceramides30.
Maintains Optimum Moisture Levels
The extent of hydration (moisturization) of infant skin represents a delicate balance between increased TEWL and increased absorption of water at the skin’s surface (leading to maceration)1,2. It is particularly important that IDD preparations should not be totally occlusive, allowing normal TEWL to occur and preventing rises in local pH. Occlusion of the skin can lead to skin barrier damage by inhibition of repair mechanisms, which are triggered by increased TEWL20. Historically, pastes made up of ≥10% powder (e.g., zinc oxide), in either water-in-oil (lipophilic) or oil-in-water (hydrophilic) vehicles, have been used. Lipophilic pastes, however, are very occlusive and can also be very difficult to remove, requiring vigorous scrubbing to remove them, causing skin damage6. This makes them particularly unsuitable for use as a daily applied preventative preparation. Water-in-oil galenics, however, are considered to be the most appropriate for IDD preparations, forming a durable and long-lasting lipid shield which protects the skin from irritants while preventing excessive water loss (Table 2).
Table 2. Table of available galenics

Contains Ingredients With Documented Safety and Benefit
Only those agents shown to be clinically efficacious and safe in infants should be included in an IDD preparation. Examples include dexpanthenol and phospholipids, which have moisturizing and skin barrier enhancing properties26,27,28,29, and vitamin B3, which inhibits faecal ureases, preventing rises in pH19.
Contains no Unnecessary Ingredients
Many infant skin care products contain components that, while not harmful, have no proven benefit in the management of IDD (Table 3). Zinc oxide, which has historically been applied as an occlusive paste, is thought to have anti-bacterial properties; however, there are no published reports from controlled studies in infants with IDD31. Furthermore, there is no evidence to suggest a primary bacterial or fungal component in the pathology of IDD6. Vitamin A (from cod liver oil) has also been suggested to ameliorate IDD progression; however, there are no published clinical studies to support this claim32.
Contains no Potentially Toxic Ingredients
While some preparations may not necessarily be toxic, substantial percutaneous absorption of particular components, such as preservatives, may be detrimental to an infant’s health. In particular, boric acid present in some formulations can cause adverse events, particularly where it is easily absorbed through a disrupted skin barrier, such as in IDD (Table 3)33,34.
Table 3. Table of ingredients which are considered to be unfavorable for a topical Irritant Diaper Dermatitis (IDD) preparation
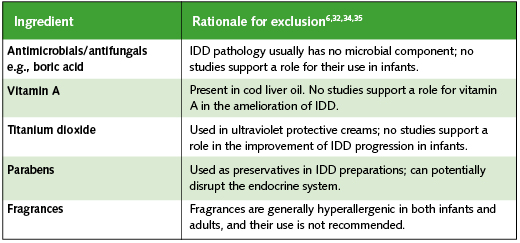

Contains no Potential Sensitizers, Such as Fragrances
The fragile nature of infant skin makes it susceptible to an array of environmental and biological allergens. Established allergens should be avoided in the formulation of an IDD preparation. Recently, the EU reported 26 fragrance components with enhanced allergenicity, including some agents readily available in IDD preparations, such as benzyl alcohol, benzyl benzoate and benzyl cinnamate (Table 3)35.
Contains no Antiseptics or Preservatives
Antiseptics were not considered by the panel to be appropriate for an IDD preparation, as micro-organisms have not been shown to have a pathogenic role in IDD6. Antimicrobial agents can alter the local composition of the protective commensal skin bacterial flora and thereby increase the risk of secondary infections6. In the prevention of IDD, the use of preservatives such as parabens was also discouraged by the panel34.
Must be Pleasant to Use
The panel believed that the focus of IDD management has now shifted from treatment to prevention. This shift may be attributed to advances in diaper technology, improvements in infant skin care and an increase in older mothers having fewer children. The properties of galenics are of particular importance in a topical preventive preparation. A preparation that is pleasant to use, easily applied, and does not require removal at each diaper change is likely to encourage compliance, thereby enhancing its protective effects. Water-in-oil ointment formulae are considered the ideal galenics as they provide a continuous protective lipophilic layer across the skin, which reduces friction and isolates the skin from irritants. (Table 2).
SUMMARY
Infant skin (<12 months), has a slightly different structure to older children’s (>12 months) skin. The SC and epidermis of infant skin is thinner and there are fewer structural collagen bundles in the dermis. The skin surface also has increased microrelief lines, which enhances the skin’s absorptive capacity2. Furthermore, a higher pH at birth and in the first months, initially due to presence of amniotic fluid and subsequently increased TEWL, may impair formation of structural lamellar lipids as well as skin barrier repair and maintenance processes1,16. IDD results primarily from an infant’s incontinence resulting in increased exposure to urine and faeces, which tend to be less solid and passed more frequently compared to older children. The more delicate SC and epidermis of infants, coupled with a susceptibility to maceration and absorptive propensity, may increase the risk of IDD6.
IDD is a multi-factorial disease which is primarily triggered by prolonged contact and interaction of urine and faeces with sensitive infant skin. Increases in pH by urine impair skin repair mechanisms and activate faecal enzymes that digest lipids and proteins of the skin, causing irritation3,6. In addition, friction occurring between the diaper and the skin, and disturbance of the SC by maceration, increase SC damage and an infant’s susceptibility to developing IDD. Although pathogenic bacteria and fungi are not primarily involved in the pathogenesis of IDD, changes in commensal microflora mediated by elevated pH raise the risk of colonization by pathogens and secondary infection, particularly by C. albicans6.
The focus of IDD management on prevention makes it important to pay careful attention to the formulation of barrier ointments. The lack of commercially available topical IDD treatments which fully and effectively address the vulnerability of an infant’s fragile skin prompted an expert panel of dermatologists and pediatricians to reach a consensus on nine standards for an ideal IDD preparation (Table 1). By ensuring that new and emerging topical IDD preparations conform to these nine consensus standards, particularly those formulations used for prevention rather than treatment in infants, the panel aimed to improve best practice and further reduce IDD incidence. The panel highlighted the need for IDD preparations to have been clinically tested in infants, to have a demonstrated safety profile, and to contain components with documented clinical benefit in IDD. In addition, agents which may have a potential sensitizing effect on the skin (e.g., fragrances) or have no proven clinical benefit, such as vitamin A, boric acid and preservatives, have also been addressed. Furthermore, although not directly discussed, the choice of galenic is also a key consideration in any new formulation and is likely to be different in formulations designed to prevent rather than treat IDD. Galenics that are easily applied and pleasant to use may be favored as preventive treatments, especially if regular application (such as at each diaper change) is required over longer periods of time.
A reduction in the sensitization potential of an IDD preparation could potentially protect infants from developing other dermatological conditions, such as AD36. However, more studies are required to establish a firm link between IDD incidence and AD prevalence. AD affects 20% of children in Northern Europe; however, paradoxically, AD does not usually present in the diaper area37. Interestingly, the pathophysiology of IDD and AD are similar, with both involving the failure of the skin barrier. However, AD also involves genetic (e.g., filaggrin gene mutations) and immunological abnormalities, which are mostly absent in IDD36. The mainstay of most dermatological treatments for IDD and AD is gentle washing, whilst application of moisturizing emollients and anti-inflammatories also form components of AD therapy.
In summary, IDD is the product of prolonged contact of urine and faeces with infant skin. However, the structural and functional differences between infant skin and that of older children increase the risk of IDD, which affects the majority of infants in the first 12 months of life. Currently available formulae are often not optimal to protect the immature skin of infants, and have the potential to sensitize the skin, which may in turn predispose infants to other allergic dermatological conditions such as AD. Nine consensus standards recommended by an expert panel of dermatologists have addressed the shortfall of current treatments by highlighting those areas which require improvement to help guide the development of the next generation of IDD treatments. These recommendations also aim to improve best practice, as prevention plays an increasingly important role in the overall management of IDD.
Correspondence to: Dr David J Atherton, Hon. Consultant in Paediatric Dermatology, Great Ormond Street Hospital for Children, London WC1N 3JH, UK. Tel. +44 (0)207 193 7568; Fax +44(0)207 692 7910;
Email david.atherton49@btinternet.com
Acknowledgements: We would also like to acknowledge the editorial assistance of Dr Stuart Marshall, formerly of Core Medica Ltd., a division of the Prime Medical Group, in the development of this manuscript.
Statement of Interest: The authors were all involved in the analyses and interpretation of the information presented in this review. The international expert panel of dermatologists and pediatricians on the optimal management of IDD was sponsored by Bayer HealthCare. The authors would like to declare the following conflicts of interest unrelated to the development of this manuscript; J. Schauber has received honoraria for lectures and/or consulting activities from Bayer HealthCare, Galderma, La Roche-Posay and Pfizer.
References
- Nikolovski J, Stamatas GN, Kollias N, Wiegand BC. Barrier function and water-holding and transport properties of infant stratum corneum are different from adult and continue to develop through the first year of life. J Invest Dermatol 2008;128:1728-1736.
- Stamatas GN, Nikolovski J, Luedtke MA, Kollias N, Wiegand BC. Infant skin microstructure assessed in vivo differs from adult skin in organization and at the cellular level. Pediatr Dermatol 2010;27:125-131.
- Hoeger PH, Enzmann CC. Skin physiology of the neonate and young infant: a prospective study of functional skin parameters during early infancy. Pediatr Dermatol 2002;19:256-262.
- Benjamin L. Clinical correlates with diaper dermatitis. Pediatrician 1987;14 Suppl 1:21-26.
- Jordan WE, Lawson KD, Berg RW, Franxman JJ, Marrer AM. Diaper dermatitis: frequency and severity among a general infant population. Pediatr Dermatol 1986;3:198-207.
- Atherton DJ. A review of the pathophysiology, prevention and treatment of irritant diaper dermatitis. Curr Med Res Opin 2004;20:645-649.
- Yadav M, Singh PK, Mittal SK. Variation in bowel habits of healthy indian children aged up to two years. Indian J Pediatr 2014;81:446-449.
- Lund C, Kuller J, Lane A, Lott JW, Raines DA. Neonatal skin care: the scientific basis for practice. J Obstet Gynecol Neonatal Nurs 1999;28:241-254.
- Putet G, Guy B, Andres P et al. Effect of Bepanthen ointment in the prevention and treatment of diaper rash on premature and full-term babies. Réalités Pédiatriques 2001;63:33-38.
- Lane AT, Drost SS. Effects of repeated application of emollient cream to premature neonates' skin. Pediatrics 1993;92:415-419.
- Horowitz P, McLeod RP, Eichenfield LF, Fowler JF, Jr., Elias PM. Skin-cleansing and care principles for special pediatric populations. Semin Cutan Med Surg 2013;32:S30-S32.
- Folster-Holst R, Buchner M, Proksch E. [Diaper dermatitis]. Hautarzt 2011;62:699-708.
- National Institute for Health and Care Excellence. Available at: https://cks.nice.org.uk/nappy-rash#!topicsummary. (Last accessed 30 January 2014).
- Gomez-Berrada MP, Gautier F, Parent-Massin D, Ferret PJ. Retrospective exposure data for baby and children care products: An analysis of 48 clinical studies. Food and Chemical Toxicology 2013;57:185-194.
- Cetta F, Lambert GH, Ros SP. Newborn chemical exposure from over-the-counter skin care products. Clin Pediatr (Phila) 1991;30:286-289.
- Hoeger PH, Schreiner V, Klaassen IA et al. Epidermal barrier lipids in human vernix caseosa: corresponding ceramide pattern in vernix and fetal skin. Br J Dermatol 2002;146:194-201.
- Warner RR, Stone KJ, Boissy YL. Hydration disrupts human stratum corneum ultrastructure. J Invest Dermatol 2003;120:275-284.
- Humphrey S, Bergman JN, Au S. Practical management strategies for diaper dermatitis. Skin Therapy Lett 2006;11:1-6.
- Stamatas GN, Tierney NK. Diaper dermatitis: etiology, manifestations, prevention, and management. Pediatr Dermatol 2014;31:1-7.
- Atherton D, Mills K. What can be done to keep babies' skin healthy? RCM Midwives 2004;7:288-290.
- Telofski LS, Morello AP, III, Mack Correa MC, Stamatas GN. The infant skin barrier: can we preserve, protect, and enhance the barrier? Dermatol Res Pract 2012;2012:198789.
- Adam R. Skin care of the diaper area. Pediatr Dermatol 2008;25:427-433.
- Ehretsmann C, Schaefer P, Adam R. Cutaneous tolerance of baby wipes by infants with atopic dermatitis, and comparison of the mildness of baby wipe and water in infant skin. J Eur Acad Dermatol Venereol 2001;15 Suppl 1:16-21.
- Atherton DJ. The aetiology and management of irritant diaper dermatitis. J Eur Acad Dermatol Venereol 2001;15 Suppl 1:1-4.
- The European Parliament. Regulation (EC) No 1223/2009 of The European Parliament and of The Council On Cosmetic Products. 2009. 1223/2009.
- Biro K, Thaci D, Ochsendorf FR, Kaufmann R, Boehncke WH. Efficacy of dexpanthenol in skin protection against irritation: a double-blind, placebo-controlled study. Contact Dermatitis 2003;49:80-84.
- Gehring W, Gloor M. Effect of topically applied dexpanthenol on epidermal barrier function and stratum corneum hydration. Results of a human in vivo study. Arzneimittelforschung 2000;50:659-663.
- Proksch E, Nissen HP. Dexpanthenol enhances skin barrier repair and reduces inflammation after sodium lauryl sulphate-induced irritation. J Dermatolog Treat 2002;13:173-178.
- Otte N, Borelli C, Korting HC. Nicotinamide - biologic actions of an emerging cosmetic ingredient. Int J Cosmet Sci 2005;27:255-261.
- Proksch E, Brandner JM, Jensen JM. The skin: an indispensable barrier. Exp Dermatol 2008;17:1063-1072.
- Bikowski, J. Update on Prevention and Treatment of Diaper Dermatitis. 2011. Last accessed on 23 April 14 A.D.
Reference Link - Davies MW, Dore AJ, Perissinotto KL. Topical vitamin A, or its derivatives, for treating and preventing napkin dermatitis in infants. Cochrane Database Syst Rev 2005;CD004300.
- See AS, Salleh AB, Bakar FA et al. Risk and Health Effect of Boric Acid. American Journal of Applied Sciences 2010;7:620-627.
- Barr L, Metaxas G, Harbach CA, Savoy LA, Darbre PD. Measurement of paraben concentrations in human breast tissue at serial locations across the breast from axilla to sternum. J Appl Toxicol 2012;32:219-232.
- Heisterberg MV, Menne T, Johansen JD. Contact allergy to the 26 specific fragrance ingredients to be declared on cosmetic products in accordance with the EU cosmetics directive. Contact Dermatitis 2011;65:266-275.
- Rahman S, Collins M, Williams CM, Ma HL. The pathology and immunology of atopic dermatitis. Inflamm Allergy Drug Targets 2011;10:486-496.
- Halkjaer LB, Loland L, Buchvald FF et al. Development of atopic dermatitis during the first 3 years of life: the Copenhagen prospective study on asthma in childhood cohort study in high-risk children. Arch Dermatol 2006;142:561-566.
